The Surprising COVID-19 Public Health Crisis That Africa Now Faces
by Jacquelyn Corley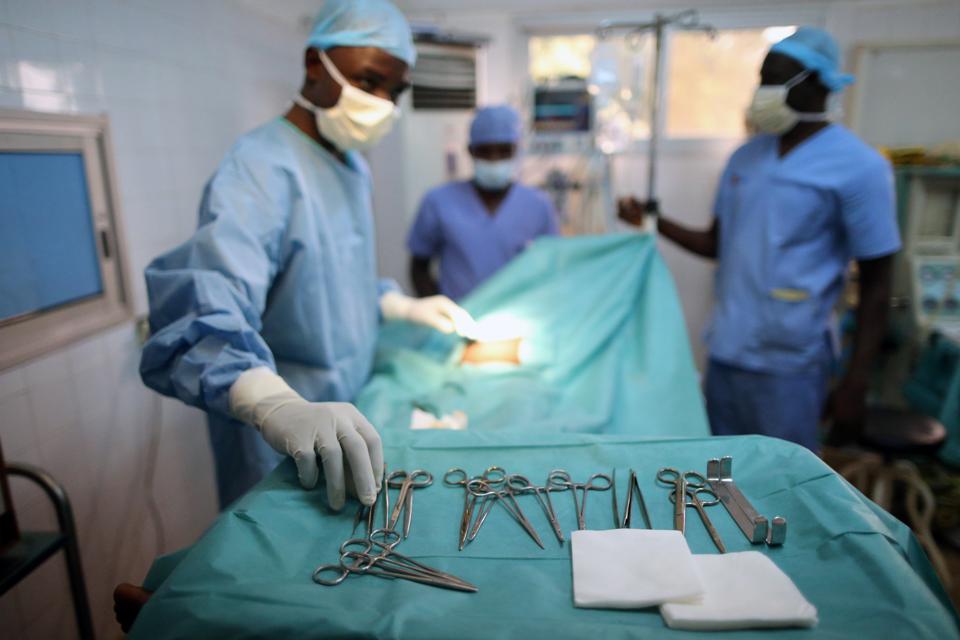
The Africa Centres for Disease Control and Prevention (Africa CDC) reports that, to date, there have been 104,279 cases of COVID-19 and 3,185 deaths, with most of these cases having occurred in the northern region of the continent. The country of South Africa has seen the most amount of cases, while Egypt and Algeria have suffered the most amount of tragic deaths.
However, even with these numbers, it seems Africa has fared better than other continents. In fact, the World Health Organization reports Africa has the least amount of cases among the most populated continents.
Although the reasons for this are not entirely clear, it is possible that one reason for the difference is that country-level data are missing, making it difficult to provide accurate and granular information. Additionally, many believe there is a lack of testing that’s playing a role in underestimating the true number of cases.
While there may be some truth to these theories, they undermine the great efforts that many of the African governments have made to aggressively impose restrictions on travel, work and social congregation. Additionally, Africans, on average, tend to be younger and less obese than their American or European counterparts, which could help to explain why there have been fewer deaths.
Regardless of whether Africa’s reported COVID-19 numbers are completely accurate, cases are undeniably on the rise throughout the continent, with some urban hot spots experiencing substantial escalations in recent weeks. Many regions in Africa have yet to reach their peak.
While every citizen and patient has had to make many sacrifices and suffer at the hands of coronavirus, one group of people has been especially harmed and forgotten: surgical patients.
For surgeons and their patients, the coming months could have devastating consequences. Thus far, elective surgical cases have been canceled or delayed in most countries. This problem is occurring around the world, but in Africa, patients are particularly vulnerable because they often seek care when their diseases are more advanced.
In the United States, for instance, many tumors and cancers are found incidentally or with only a minimal amount of symptoms. Patients can seek treatment at these early stages and have the greatest chance of a good prognosis. Alternatively, in many countries in Africa, patients may not have the same access to health care, so tumors and cancers are often not found until much later, so waiting to receive treatment after a diagnosis can mean the difference between life and death.
Another key difference between African countries and many European and North American nations is that many of their citizens rely on public transportation. With strict lockdowns, buses, trains and commuter cars have gone into hibernation, making it difficult for patients and healthcare workers alike to travel to hospitals.

Even prior to the pandemic, many African regions were already facing deficits in surgical, anesthesia and obstetric workforce. Now, numerous healthcare providers have been re-assigned to other departments that are desperately in need of manpower, such as intensive care units and emergency departments. Further, precious resources that are necessary for safe surgeries, such as blood banks, oxygen and ventilators, have been diverted to COVID-19 units.
COVID-19 has also greatly disrupted surgical training and education at a time when these processes have finally started to gain momentum. Of all subjects, surgery does not translate well to current and available virtual platforms, given its focus on three-dimensional anatomy and procedural training.
Education has suffered not only from lack of elective cases, but also from adjustments to boards and qualifying examinations. The College of Medicine of South Africa has canceled or postponed some of their first semester oral examinations. The College of Surgeons of East, Central and Southern Africa has been forced to make many modifications to its written examinations, and there is concern for further cancellations down the road.
Professor Abebe Bekele is a general and thoracic surgeon and the founding dean of the University of Global Health Equity in Butaro, Rwanda. In an interview conducted with me this past week, he explained, “COVID caught us unprepared. In this region, undergraduate medical education is completely interrupted, residency programs are really struggling and surgical services are hit hard.”
Surgery, anesthesia and obstetric care are integral to all facets of providing healthcare, including tumor removal or biopsy for cancer care, cesarean section during pregnancies, burns and traumas. In recent decades, Africa has slowly experienced a growth in delivery of these services across the continent, which is evidenced by the growing interest in engineering National Surgery, Obstetric, and Anesthesia Plans. But this growth will almost certainly be hindered by the new oppressive COVID-19 developments. The only question is, for how long?
For now, it seems all health care providers can do is continue to support patients as much as possible by getting them to operating rooms as quickly as COVID-19 will allow. In the long run, aggressively pushing forward an agenda that calls for surgical system strengthening is key to not only combat the havoc of this pandemic but also to prevent death and suffering during the next one.
Educational initiatives need to be prioritized and innovative solutions are the only way to create a capable surgical, anesthesia and obstetric workforce. To that end, Dean Bekele adds, “We need to build a robust digital learning infrastructure as soon as possible, otherwise the COVID epidemic is bound to leave a big and ugly academic scar.”